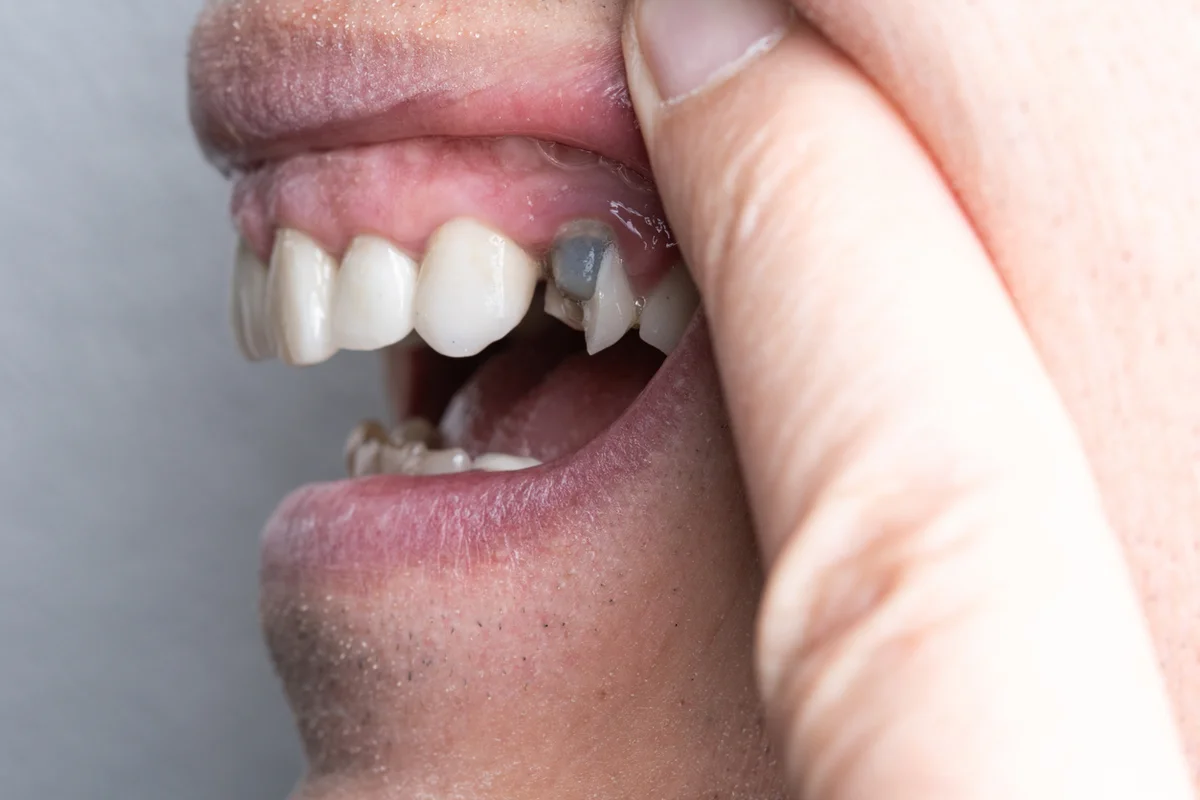
Dental Implant Infection Signs: When to Call Your Dentist
Dental Implant Infection Signs: When to Call Your Dentist
Overview
Dental implants can restore chewing, comfort, and confidence, but like any procedure that involves healing tissue, there is a small risk of infection. Knowing what is normal after surgery versus what could signal a problem is the fastest way to protect your result.
This dental implant infection signs guide explains the most common symptoms to watch for, when to call your dentist, what early treatment often looks like, and how infections can sometimes contribute to implant complications. If you are worried your implant may not be healing properly, you can also review next-step options for problem implants here: failed implant repair in Roseville
Key Takeaways
Mild swelling and soreness early on can be normal, but worsening symptoms after initial improvement can be a red flag.
Common infection signs include increasing pain, swelling, redness, pus or bad taste, fever, and bleeding that does not improve.
A loose implant or a bite that suddenly feels different should be checked quickly.
Early evaluation and treatment can often prevent small issues from turning into major complications.
What’s Normal After Dental Implant Surgery vs What’s Not
It helps to separate normal healing from warning signs. Many patients feel:
mild to moderate soreness for a few days
swelling that peaks early and then gradually improves
minor bruising
mild bleeding that reduces within the first day
What is not typical is a pattern where symptoms get better and then suddenly get worse, or where pain and swelling steadily increase after the first few days.
A quick rule of thumb
If you are improving day by day, that usually supports normal healing. If you are getting worse, especially after day 3, it is time to call your dentist.
Dental Implant Infection Signs to Watch For
Below are the most important signs that may indicate infection or a healing complication. Not every symptom automatically means infection, but these are strong reasons to get evaluated.
1) Persistent or worsening pain
Some discomfort is expected after surgery. Pain that:
increases after the first few days
becomes sharp or throbbing
does not respond to recommended pain relief
wakes you at night or keeps escalating
can suggest infection or another issue that needs attention.
2) Swelling, redness, or warmth that increases
Swelling that peaks early and then improves is common. Swelling that keeps growing, feels hot, or spreads to nearby areas may indicate infection or inflammation that is not settling.
3) Pus, drainage, bad taste, or bad odor
Drainage from around the implant site is one of the most specific warning signs. Pus, a foul taste, or persistent odor can indicate bacterial activity that should be treated promptly.
4) Fever, chills, or feeling generally unwell
A fever after surgery can be a sign your body is fighting an infection. If you feel sick, shaky, or feverish, contact your dental office quickly.
5) Bleeding that does not improve
Light bleeding early can be normal. Bleeding that continues, restarts heavily, or worsens with swelling may signal inflammation, tissue irritation, or infection.
6) Gum changes around the implant
Watch for:
gums that look increasingly red or puffy
gums that bleed easily when gently cleaned
gum recession exposing more of the implant area
tissue that looks grayish, unusually tender, or ulcerated
These changes can be early signs of trouble, especially if combined with pain or discharge.
7) A loose implant, loose crown, or sudden bite change
An implant should not feel loose once integrated. A crown may loosen from a screw or cement issue, which is often fixable, but it still needs evaluation. A sensation that something is moving, wobbling, clicking, or that your bite suddenly feels off should be checked right away.
Why Infections Happen Around Dental Implants
Infections typically start when bacteria accumulate in a way that overwhelms the body’s ability to control inflammation. This can happen:
during early healing if the site becomes contaminated
later if plaque builds up around the implant and gumline
if there is leftover cement under the gumline in some cement-retained restorations
when systemic or lifestyle factors increase inflammation risk
There are two common inflammatory conditions clinicians look for:
Peri-implant mucositis: inflammation of the gums around an implant without bone loss, often reversible when treated early.
Peri-implantitis: inflammation with bone loss around an implant, more serious and may threaten implant stability if untreated.
Risk Factors That Increase Infection Risk
Some risk factors are controllable, others are not, but knowing them helps you and your dental team plan better.
Poor oral hygiene or plaque buildup
Implants need daily cleaning just like natural teeth. Plaque around the gumline can trigger inflammation that progresses if ignored.
Smoking or nicotine exposure
Smoking can slow healing and increase inflammation. It also makes gum tissue more vulnerable to infection and delayed recovery.
Diabetes or immune-related conditions
Uncontrolled diabetes and immune suppression can reduce healing capacity and increase infection risk. Stable medical management improves predictability.
Gum disease history
If you have a history of periodontal disease, you may have a higher baseline risk for peri-implant inflammation, which makes maintenance and recall visits especially important.
Excess bite forces or grinding
Overload does not cause infection by itself, but it can irritate tissues, complicate healing, and make an inflamed site harder to stabilize. Many patients benefit from bite adjustments or a night guard when needed.
What to Do If You Notice Infection Signs
If you suspect infection, the most important step is to act early.
Step 1: Contact your dentist promptly
Call the office and describe:
what you feel (pain, swelling, discharge, fever)
when it started
whether symptoms are improving or worsening
whether you can chew comfortably or feel looseness
If you have a fever, facial swelling, or difficulty swallowing or breathing, seek urgent care immediately.
Step 2: Do not “wait it out” if symptoms are worsening
Implant infections can sometimes progress from mild inflammation to deeper tissue involvement. Early evaluation usually means simpler treatment.
Step 3: Follow professional instructions closely
Your dentist may recommend:
gentle cleaning instructions
specific rinses
medications when appropriate
a follow-up visit to check response
Avoid starting leftover antibiotics on your own. Incorrect use can mask symptoms without solving the cause.
Step 4: Track changes
Note whether swelling is spreading, whether pain changes with chewing, and whether discharge is present. This helps your dentist assess severity and next steps.
What Treatment Often Looks Like
Treatment depends on whether the problem is early post-op infection, gum inflammation, or peri-implant disease later on.
Common professional steps can include:
evaluation of the implant, gums, bite, and restoration fit
cleaning around the implant and removing plaque or irritants
checking for trapped cement if a crown was cemented
targeted therapy such as antimicrobial rinses or antibiotics when clinically indicated
deeper decontamination of the implant surface if peri-implantitis is present
surgical intervention in advanced cases
If an implant is failing or bone support is compromised, your dentist may discuss additional options. If you want to understand what happens when an implant does not heal as expected, see: failed implant repair in Roseville
When to Seek Immediate Care
Call your dentist urgently or seek emergency care if you experience:
rapidly increasing facial swelling
fever with worsening pain
pus with spreading swelling
trouble swallowing, breathing, or opening your mouth
uncontrolled bleeding
severe pain that is escalating rather than improving
These symptoms should not be monitored at home.
How to Reduce Infection Risk
You cannot control everything, but you can meaningfully reduce risk with daily habits and follow-ups.
Keep hygiene simple and consistent
brush gently at the gumline
clean between teeth daily using floss, interdental brushes, or a water flosser if recommended
use prescribed rinses exactly as directed, more is not always better
Do not smoke during early healing if possible
Even a temporary break during the early healing period can support better tissue recovery.
Attend maintenance visits
Professional cleanings and checks help catch early inflammation before it becomes serious. This is one of the biggest long-term protectors for implants.
Follow diet and bite restrictions
After surgery, avoid hard foods and chewing aggressively on the surgical side until cleared. For full-arch temporaries, diet restrictions are especially important to reduce overload.
Your Questions Answered
Q1: How soon can an infection start after implant surgery?
An infection can begin within days if bacteria enter the healing site, but issues can also develop weeks or months later if inflammation builds around the implant. Early infections often show increasing pain, swelling, and sometimes drainage. Later infections may present as bleeding gums, bad taste, or gum tenderness that slowly worsens.
Q2: How do I know if my symptoms are normal healing or an infection?
Normal healing typically improves day by day, even if you still feel sore. Infection is more likely when symptoms worsen after initial improvement, or when you see pus, a persistent bad taste, fever, or spreading swelling. When in doubt, a quick check is safer than guessing.
Q3: Is bleeding around an implant always a sign of infection?
Not always. Mild bleeding right after surgery can be normal, and gums can bleed if they are irritated during cleaning. Bleeding that increases, persists, or occurs with swelling, pus, or pain is more concerning and should be evaluated.
Q4: What if I notice a bad taste or odor near the implant?
A bad taste or odor can be a sign of trapped debris, gum inflammation, or infection, especially if it persists despite gentle hygiene. If it is paired with discharge, swelling, or tenderness, call your dentist. Early treatment is usually simpler than delayed care.
Q5: Can an infected implant be saved?
Sometimes, yes. Mild inflammation or early infection can often be managed with professional cleaning, targeted therapy, and close follow-up. Advanced peri-implantitis with significant bone loss is more complex, and treatment depends on how much support remains and how the implant responds.
Q6: What are signs an implant might be failing?
Warning signs can include persistent pain, repeated swelling, drainage, deep gum pockets, or a sense that the implant or crown is loose. A bite that suddenly feels different can also be a clue. If you suspect implant failure, it’s important to get evaluated promptly because early action can preserve more options.
Conclusion
Knowing what to watch for is one of the best ways to protect your investment. This dental implant infection signs guide covers the most important red flags, pain that worsens, swelling that increases, pus or bad taste, fever, gum changes, and looseness. If you notice these symptoms, don’t wait, call your dentist and get the site evaluated.
If you are worried an implant is not healing properly, or you suspect a serious complication, you can review next-step options for problem implants here: failed implant repair in Roseville
Key Term Definitions
TERM: Peri-implant mucositis
DEFINITION: Inflammation of the gum tissue around an implant without bone loss. It is often reversible with professional cleaning and improved home care.
TERM: Peri-implantitis
DEFINITION: Inflammation and infection around an implant with progressive bone loss. It can threaten implant stability if untreated.
TERM: Osseointegration
DEFINITION: The process where jawbone bonds to the implant surface after placement. This bonding creates long-term implant stability.
TERM: Implant crown
DEFINITION: The visible tooth portion attached to an implant, designed to restore chewing and appearance. A crown may be screw-retained or cement-retained depending on the plan.
TERM: Implant failure
DEFINITION: A situation where an implant does not integrate properly or loses stability over time. It can be related to infection, bone loss, overload, or healing factors.
TERM: Surgical site
DEFINITION: The area where the implant was placed and tissues are healing. Protecting the site from pressure and irritation reduces complication risk.
TERM: Antimicrobial rinse
DEFINITION: A prescribed mouth rinse that helps reduce bacterial load during healing or treatment. It should be used only as directed to avoid irritation.
Ready to Transform Your Smile?
Schedule your free consultation today and discover how dental implants can change your life.

