Peri-Implantitis Treatment: How Gum Infection Around Implants Is Managed
Peri-Implantitis Treatment: How Gum Infection Around Implants Is Managed
Overview
Dental implants are a durable, natural-looking way to replace missing teeth, but they still require healthy gums and consistent maintenance. One of the most important complications to understand is peri-implantitis, an inflammatory infection around a dental implant that can lead to bone loss and, in advanced cases, implant failure. Knowing the right peri implantitis treatment options helps you recognize problems early, seek timely care, and protect your long-term results.
Key Takeaways
• Peri-implantitis is inflammation and infection around an implant that can cause bone loss.
• Early treatment improves the chance of stabilizing the implant and preventing progression.
• Treatment ranges from professional cleaning and antimicrobial care to surgical therapy in advanced cases.
• Prevention depends on daily cleaning, regular professional maintenance, and risk-factor control.
What Is Peri-Implantitis?
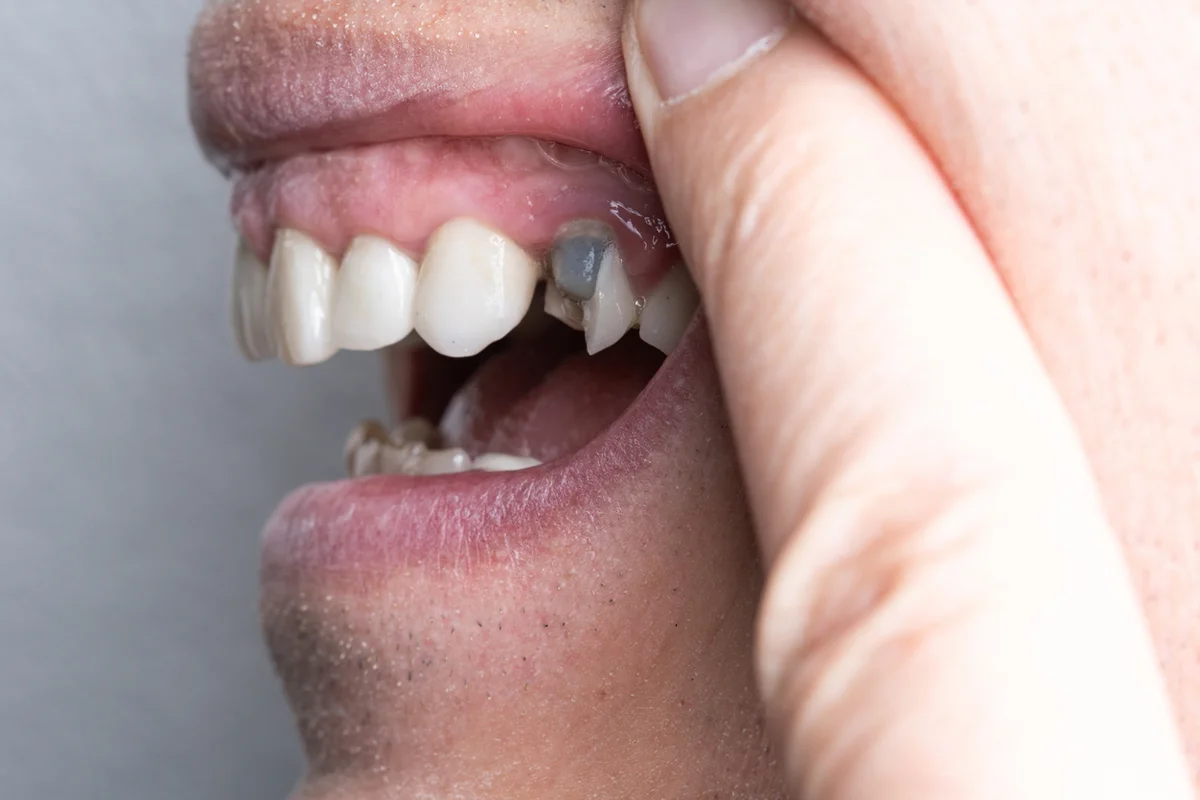
Peri-implantitis is an inflammatory condition affecting the gum and supporting bone around a dental implant. It often starts with plaque and bacterial buildup at the gumline. Over time, inflammation can deepen, leading to bone loss around the implant.
Common signs include:
• Bleeding when brushing or flossing around the implant
• Redness, swelling, or tenderness of the gum tissue
• Bad taste or odor, sometimes with pus
• Deepening “pockets” around the implant when measured by a dentist
• In advanced cases, discomfort when chewing or a feeling of looseness
Peri-implantitis is serious because bone loss can reduce implant stability. The earlier it is identified, the more conservative the treatment can be.
Peri-Implant Mucositis vs Peri-Implantitis
These two terms are often confused, and the difference matters for treatment planning.
Peri-implant mucositis
This is inflammation of the soft gum tissue around an implant without bone loss. It is similar to gingivitis around natural teeth. The good news is that mucositis is often reversible with professional cleaning, improved home care, and consistent follow-ups.
Peri-implantitis
This includes inflammation plus progressive bone loss. It is more complex and may require a combination of cleaning, antimicrobial therapy, correction of mechanical factors, and sometimes surgical treatment. When people search for peri implantitis treatment options, they are usually dealing with this more advanced condition or trying to prevent it from reaching that stage.
Causes and Risk Factors
Peri-implantitis typically results from a combination of bacterial plaque and contributing risk factors. Understanding these helps guide both treatment and prevention.
Plaque and bacterial biofilm
Just like natural teeth, implants can accumulate plaque. If plaque stays at the gumline, inflammation can build and deepen.
Poor oral hygiene or difficult-to-clean implant design
Some restorations are harder to clean due to shape, spacing, or how they sit on the gum. If flossing and interdental cleaning are not effective, inflammation risk increases.
History of gum disease
Patients with past or active periodontal disease often have a higher risk of implant inflammation. This does not mean implants are not possible, but it usually means maintenance needs to be stricter.
Smoking and nicotine use
Smoking and nicotine reduce blood flow and impair healing. They are consistently linked with higher complication risk and poorer gum outcomes around implants.
Uncontrolled diabetes and other systemic factors
Uncontrolled diabetes can increase infection risk and slow healing. Other medical conditions that affect immune response can also impact gum stability.
Excessive bite forces and implant overload
Grinding and clenching, bite imbalance, or poorly distributed forces can contribute to bone stress and tissue breakdown. Mechanical overload does not cause infection by itself, but it can worsen inflammation and accelerate bone loss when plaque is present.
How Peri-Implantitis Is Diagnosed
Diagnosis involves more than a quick look. A thorough evaluation helps determine severity and the most appropriate treatment approach.
Typical diagnostic steps include:
• Clinical exam: checking gum inflammation, bleeding, pus, gum recession, and tenderness
• Probing measurements: measuring pocket depths around the implant and checking for bleeding on probing
• Radiographs: X-rays to assess bone levels and compare with past images
• Occlusion assessment: evaluating bite forces and signs of overload
• Medical history review: identifying smoking, diabetes control, medications, and other risk factors
A precise diagnosis is important because treatment depends on whether bone loss is present and how rapidly the condition is progressing.
Peri Implantitis Treatment Options
Effective care aims to remove bacterial buildup, reduce inflammation, and stop bone loss. The best plan depends on severity, implant position, restoration design, and patient risk factors.
Treatment options by severity
This approach makes it easier to understand what your dentist is likely to recommend.
Mild to early disease
Goal: reduce inflammation, improve cleaning access, stabilize gum tissue
Common approaches:
• professional debridement and polishing
• targeted antimicrobial rinses or gels as appropriate
• home-care upgrades with the right tools
• closer maintenance intervals for monitoring
Moderate disease with measurable bone loss
Goal: reduce bacterial load, address contributing factors, slow or stop progression
Common approaches:
• deeper professional debridement around the implant
• antimicrobial therapy, sometimes localized delivery based on clinical judgment
• adjustment of the restoration if it traps plaque or blocks cleaning
• bite adjustment if overload is suspected
• strict follow-up to evaluate response
Advanced disease with significant bone loss
Goal: access and thoroughly clean infected areas, attempt regeneration when appropriate, or remove the implant if it cannot be stabilized
Common approaches:
• surgical access therapy to clean implant surfaces and infected tissue
• regenerative procedures, bone grafting in selected cases
• resective approaches in some cases to reduce pocket depth and improve cleanability
• implant removal as a last resort when prognosis is poor
Non-surgical treatments
Non-surgical care is often the first step, especially when the condition is caught early or when inflammation is mild.
Professional cleaning and debridement
This is a deep, implant-safe cleaning focused on removing plaque and hardened deposits around the implant. Your clinician may use special instruments designed to avoid damaging implant surfaces. The goal is to reduce bacterial biofilm and calm gum inflammation.
Antimicrobial therapy
This may include topical antimicrobial agents placed around the implant and, in specific cases, systemic antibiotics. Antibiotics are not always necessary and are usually considered when there are clear signs of infection, swelling, pus, or deeper pocketing that suggests bacterial invasion beyond what cleaning alone can address.
Laser therapy
Laser therapy may be used as an adjunct in some practices to help reduce bacteria and inflamed tissue. It is not a universal “one-step cure,” but it can be part of a broader plan that includes cleaning, improved home care, and follow-up monitoring.
Maintenance programs and supportive therapy
Maintenance is where long-term success is protected. A good plan includes:
• more frequent professional cleanings in higher-risk patients
• evaluation of pocket depths and bleeding at each visit
• reinforcement of home-care technique
• early intervention at the first sign of recurrence
Surgical treatments
Surgery is typically considered when non-surgical therapy does not control inflammation or when there is significant bone loss.
Flap surgery and implant surface decontamination
Flap surgery involves gently lifting gum tissue to access deeper infected areas. This allows thorough cleaning of inflamed tissue and improved access to the implant surface. The clinician may also reshape the area to improve future cleaning access.
Bone grafting and regenerative procedures
In selected cases, bone grafting may be used to rebuild lost bone support. Not every peri-implantitis case is a good candidate for regeneration, success depends on defect shape, implant position, and infection control. Your clinician should explain the expected benefit, limitations, and likelihood of stability.
Implant removal
When the implant has extensive bone loss, persistent infection, or mobility, removal may be the most predictable option. While that can feel discouraging, it can also be the safest path to restore health and plan a better long-term solution, sometimes with future re-implantation after healing.
What to Expect During Treatment
Treatment is often staged. Your provider may start with conservative therapy and reassess response before recommending surgery.
A typical journey might look like:
Diagnosis with probing and X-rays
Non-surgical debridement and antimicrobial support
Home-care upgrades and risk-factor reduction
Re-evaluation in several weeks
Surgical therapy if inflammation and pocketing persist
Structured maintenance schedule long-term
The key is follow-through. Peri-implantitis is rarely solved with a single appointment.
Recovery and Follow-Up
Recovery depends on the treatment type.
After non-surgical therapy, most people return to normal routines quickly. You may have mild gum soreness and sensitivity, especially if deeper cleaning was needed.
After surgical therapy, you may experience swelling and tenderness for several days. Your dentist may recommend:
• a soft-food diet briefly
• careful cleaning instructions around the surgical site
• antiseptic rinses
• follow-up visits to check healing and gum response
Healing is not just about comfort. Follow-up visits help confirm whether inflammation is decreasing and whether pockets are becoming more stable.
Prevention of Peri-Implantitis
Prevention is often the most cost-effective and predictable strategy. Even if you have already had peri-implantitis treated, prevention reduces the chance of recurrence.

Daily oral hygiene habits that matter
• Brush twice daily with attention to the gumline
• Use interdental brushes or floss tools designed for implants and bridges
• Consider a water flosser if spacing or restoration design makes cleaning difficult
• Clean gently but thoroughly, implants need consistent plaque control
Professional maintenance
Regular check-ups and cleanings help detect early mucositis before it becomes peri-implantitis. Many implant patients benefit from more frequent professional maintenance, especially if they have a history of gum disease.
Reduce risk factors
• Quit smoking or reduce nicotine use significantly
• Keep diabetes well controlled
• Address grinding or clenching with a night guard if recommended
• Correct bite imbalances that overload the implant
Lifestyle Changes to Support Gum and Bone Health
Lifestyle matters because the mouth is part of the body, and healing depends on overall health.
• Balanced diet: Protein supports healing, and nutrients like calcium and vitamin D support bone health.
• Hydration: Helps maintain saliva flow and reduces bacterial buildup.
• Stress management: Chronic stress can influence immune response and hygiene consistency, both relevant for gum stability.
• Sleep: Good sleep supports recovery and inflammation control.
When to Call a Dentist Right Away
Seek care promptly if you notice:
• persistent bleeding around the implant
• swelling that worsens or returns after improving
• pus, bad taste, or foul odor near the implant
• pain that increases after a few days rather than improving
• a feeling that the implant or crown is loose
• gum recession exposing more of the implant surface
Early care often means simpler treatment.
Your Questions Answered
Q1: What are the symptoms of peri-implantitis?
Symptoms commonly include redness, swelling, bleeding when cleaning, and tenderness around the implant. Some people notice bad breath, a bad taste, or pus near the gumline, especially in more active infection. As the condition progresses, you may feel discomfort when chewing or notice changes in the way the implant crown feels.
Q2: How is peri-implantitis diagnosed?
Diagnosis usually involves a clinical exam with probing to measure pocket depths and check for bleeding or pus. Your dentist will also use X-rays to assess bone levels and compare them with earlier images if available. A good diagnosis also includes checking bite forces and reviewing risk factors like smoking, diabetes control, and history of gum disease.
Q3: What are the non-surgical treatment options for peri-implantitis?
Non-surgical options typically include professional implant-safe cleaning, debridement to remove plaque and deposits, and tailored home-care guidance to improve daily plaque control. Antimicrobial therapy may be added as a rinse, gel, or localized treatment depending on inflammation and infection signs. Some practices also use laser therapy as an adjunct, but results are best when combined with consistent maintenance and improved cleaning access.
Q4: When is surgery necessary for peri-implantitis?
Surgery is often considered when deeper pockets persist, bone loss is significant, or inflammation does not resolve after thorough non-surgical therapy. Surgical access allows deeper cleaning and removal of infected tissue where instruments cannot reach effectively without lifting the gum. In selected cases, your dentist may recommend regenerative procedures, but the suitability depends on anatomy, infection control, and overall prognosis.
Q5: Can peri-implantitis be prevented?
Yes, prevention is often possible, especially when early inflammation is caught at the mucositis stage. Daily plaque control, implant-friendly cleaning tools, and regular professional maintenance are the foundation. Avoiding smoking, controlling diabetes, and addressing grinding or bite overload further reduce risk and support long-term implant health.
Q6: What lifestyle changes can support oral health and lower risk?
A balanced diet supports gum healing and bone health, and good hydration helps reduce bacterial buildup. Stress management and adequate sleep support immune function and reduce inflammation, which can influence gum stability. If you smoke, reducing or quitting nicotine is one of the most meaningful changes you can make for implant longevity.
Conclusion
Peri-implantitis can threaten dental implant success, but it is manageable when caught early and treated with a structured plan. The best outcomes come from accurate diagnosis, staged care, and a long-term maintenance approach that addresses both bacterial plaque and contributing risk factors. Understanding the full range of peri implantitis treatment options empowers you to act quickly, protect your investment, and preserve your oral health.
If you suspect infection around an implant, or if you want an expert assessment of gum health and bone stability, schedule a consultation with Fusion Dental Implants. Early evaluation can make treatment simpler and outcomes more predictable.
Key Term Definitions
TERM: Peri-Implantitis
DEFINITION: Peri-implantitis is an inflammatory condition that occurs around a dental implant, characterized by the presence of infection and inflammation in the gum and supporting bone. This condition typically begins with the accumulation of plaque and bacteria, leading to symptoms such as gum swelling, redness, and potential bone loss if left untreated.
TERM: Peri-Implantitis Treatment Options
DEFINITION: Peri-implantitis treatment options refer to the various methods employed to manage and resolve the inflammatory infection surrounding a dental implant. These options can range from non-surgical approaches, such as professional cleaning and the use of antimicrobial agents, to more invasive surgical procedures in cases of advanced infection.
TERM: Bone Loss
DEFINITION: Bone loss is the gradual reduction of bone density and structure, which can occur as a result of inflammation or infection around dental implants. In the context of peri-implantitis, bone loss can compromise the stability of the implant, potentially leading to its failure if not addressed promptly.
TERM: Professional Cleaning
DEFINITION: Professional cleaning is a dental procedure performed by a qualified dental hygienist or dentist that involves the thorough removal of plaque, tartar, and bacteria from the surfaces of teeth and around implants. This treatment is crucial for maintaining gum health and preventing conditions like peri-implantitis.
Ready to Transform Your Smile?
Schedule your free consultation today and discover how dental implants can change your life.

